By Jessica Walsh
In what may be a sign of the never-ending quest to give simple medical problems complex names, many doctors are now regularly diagnosing gastroesophageal reflux disease (GERD). In the old days, we called this aliment hiatal hernia or esophageal reflux—or simply heartburn.
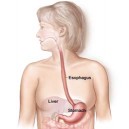
Whatever the name, GERD is what happens when stomach contents leak upstream into the esophagus, the muscular tube linking the mouth to the stomach. Typical symptoms include a burning sensation in the lower chest and an acid taste in the mouth.
The condition can be disabling, and severe cases can even lead to esophageal cancer. Luckily, most cases can be controlled with lifestyle modifications, drugs and in some extreme cases—surgery.
The first line of treatment for GERD is dietary modification. This involves avoiding foods known to trigger reflux. These include chocolate, coffee (including decaf), peppermints and other mints, citrus fruits and spicy or fatty foods. Drinking alcohol and smoking also promote reflux.
Certain medicines make worse. These include the asthma drug theophylline, anti-inflammatory drugs like aspirin and ibuprofen, tricyclic antidepressants like amitriptyline (Elavil) and calcium channel blockers, which are used to treat heart disease and high blood pressure.
If you have GERD and are taking any of these drugs, ask your doctor about substituting another drug.
Anything that pushes on the belly encourages stomach acid to “backwash” into the esophagus. Tight clothing can do it. So avoid being overweight or even eating too much at a time.
When you’re standing or sitting, gravity tends to keep stomach contents from moving upstream. For this reason, people prone to GERD should avoid lying down after eating, and should not eat or drink anything—even a glass of water—for a couple of hours before going to bed. Some people benefit by elevating the head of the mattress with a foam wedge or placing the headboard on wooden blocks.
If lifestyle modification fails to bring relief the first line of drug therapy for GERD is antacids. They bring quick relief by coating the esophagus and helping neutralize the stomach acid blocker, such as Zantac 75 or Pepacid AC. If these drugs don’t help, ask your doctor about prescription-strength versions. Tagamet, a similar drug, is no more likely to interact with drugs.
The last resort for controlling GERD is usually surgery. In one procedure, called fundoplication, the surgeon wraps the upper portion of the stomach around the lower end of the esophagus. This operation can be very effective—although it isn’t always final and symptoms may recur years later.
If you go this route, be sure to ask your doctor about laparoscopic techniques. They require smaller incisions and afford faster recovery than conventional surgery. Check the surgeon’s track record, too. Some have much better luck than others.
Note: Jessica Walsh is an internist who practices medicine in Ontario, Canada. She wrote this piece, especially for CSMS Magazine.
Also see The “Healthy” Diet that can potentially be bad for you
Lemon and Lime: nature’s sour fruits
Peach: The Healthy Persian Fruit
Watermelon: nature’s healthiest fruit
Avocados: nature’s health conscience fruit
Eating right is all that matters,not how much
Have you tried grilled turkeyburgers with avocado mayonnaise?